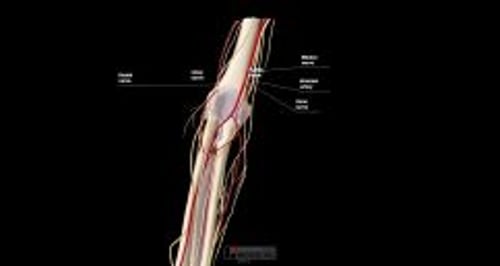
A traction-countertraction technique is recommended to reduce a posterior elbow dislocation. Procedural sedation and analgesia (PSA) is usually required.
(See also Overview of Dislocations and Elbow Dislocations.)
Indications for Posterior Elbow Dislocation Reduction
Posterior dislocation of the elbow
Reduction should be attempted soon (eg, within 30 minutes) after the diagnosis is made. An associated neurovascular deficit warrants immediate reduction.
Open dislocations require surgery, but closed reduction techniques and splinting should be performed as interim treatment if the orthopedic surgeon is unavailable and a neurovascular deficit is present.
Contraindications to Posterior Elbow Dislocation Reduction
Complicated dislocation (dislocation with associated fractures) or neurovascular compromise, because the procedure itself may increase injury severity
In these situations, reduction, if performed, should be performed in consultation with an orthopedic surgeon.
Complications for Posterior Elbow Dislocation Reduction
Brachial artery injury is uncommon but may occur in the absence of fractures.
Nerve injury (median and ulnar nerves) is uncommon and can be due to local swelling, entrapment, or traction during the reduction.
Equipment for Posterior Elbow Dislocation Reduction
Materials and personnel required for procedural sedation and analgesia (PSA)
Intra-articular anesthetic (eg, 5 mL of 2% lidocaine, 10-mL syringe, 5 cm (2-inch) 20-gauge needle), antiseptic solution (eg, chlorhexidine, povidone iodine), gauze padsIntra-articular anesthetic (eg, 5 mL of 2% lidocaine, 10-mL syringe, 5 cm (2-inch) 20-gauge needle), antiseptic solution (eg, chlorhexidine, povidone iodine), gauze pads
Posterior arm splint materials and sling
One assistant is needed.
Additional Considerations for Posterior Elbow Dislocation Reduction
Associated ligamentous injuries (lateral and medial ulnar collateral ligaments) are common with elbow dislocations and can simulate clinical findings of posterior elbow dislocations; therefore, pre- and post-procedure radiographs are recommended.
Posterior elbow dislocations are painful; IV analgesia may be given prior to radiographs, and procedural sedation and anesthesia—alone or combined with intra-articular anesthesia—is usually given for the procedure.
Regional anesthesia may be used (eg, axillary nerve block) but has the disadvantage of limiting post-reduction neurologic examination.
Relevant Anatomy for Posterior Elbow Dislocation Reduction
Due to collateral circulation around the elbow, presence of distal pulses does not exclude vascular injury. Angiography is needed if signs of arterial injury (eg, pallor, pain, cyanosis, soft tissue expansion [possible hematoma]) are present.
Positioning for Posterior Elbow Dislocation Reduction
Place the patient prone on the stretcher with the elbow flexed and the forearm dangling over the edge of the stretcher.
Raise the stretcher to your pelvic level; lock the wheels of the stretcher.
Alternative positioning: If the patient cannot lie prone, or if the prone position reduction attempt fails, perform reduction with the patient supine or reclining.
Step-by-Step Description for Elbow Dislocation Reduction
Neurovascular examination
Perform a pre-procedure neurovascular examination of the affected arm, and repeat the examination after each reduction attempt. Assess the following:
Distal pulses, capillary refill, and temperature (for coolness, suggesting brachial artery injury)
Light touch sensation of the thenar and hypothenar eminences (median and ulnar nerves), and dorsum of the 1st web space (radial nerve)
Wrist flexion and pronation, thumb-index finger apposition ("OK" gesture), and finger flexion against resistance (median nerve)
Finger abduction against resistance (ulnar nerve)
Wrist and finger extension against resistance (radial nerve)
Analgesia
Procedural sedation and anesthesia (PSA) is usually given. Intra-articular analgesia may be given in addition (eg, beforehand), to permit lower PSA dosing. To administer intra-articular analgesia:
Locate the needle insertion site, in the center of a triangle formed by the head of the radius, the lateral olecranon, and the lateral humeral epicondyle.
Swab the area with antiseptic solution, and allow the antiseptic solution to dry for at least 1 minute.
Optional: Place a skin wheal of local anesthetic (≤ 1 mL) at the site.
Insert the intra-articular needle perpendicular to the skin, aiming toward the medial epicondyle; apply suction to the syringe plunger and advance the needle 1 to 2 cm or until blood is aspirated.
If any blood is aspirated from the joint, hold the needle hub motionless, switch to an empty syringe, aspirate all of the blood, and re-attach the anesthetic syringe.
Inject 3 to 5 mL of anesthetic solution (eg, 2 % lidocaine).Inject 3 to 5 mL of anesthetic solution (eg, 2 % lidocaine).
Wait for analgesia to occur (up to 15 to 20 minutes) before proceeding.
Administer procedural sedation and analgesia.
Reduce the elbow—prone position
Place the patient prone, with the forearm dangling over the side of the stretcher.
Have an assistant stabilize the affected upper arm against the stretcher, wrapping both hands around the distal humerus and using the thumbs to apply pressure to distract the posterior aspect of the olecranon.
Apply steady downward traction to the forearm while maintaining flexion of the elbow. Signs of a successful reduction usually include a lengthening of the forearm and a perceptible “clunk.”
If the joint is not reduced, ask the assistant to lift the humerus while maintaining the downward pressure on the olecranon while you attempt to further flex the elbow.
Maintain these forces on the elbow for up to 10 minutes if necessary.
If the initial approach does not reduce the dislocation, consider using a traction-countertraction technique with the patient supine.
Reduce the elbow — supine position
Place the patient in the supine position and have an assistant stabilize the humerus with both hands.
Grasp the patient's wrist, keep it supinated, apply steady axial traction, and slightly flex the elbow to keep the muscles of the triceps loose.
Maintain these forces on the elbow for up to 10 minutes if necessary.
Signs of a successful reduction usually include a lengthening of the forearm and a perceptible “clunk.”
Aftercare for Posterior Elbow Dislocation Reduction
Perform a post-procedure neurovascular examination. A post-procedure neurovascular deficit warrants emergent orthopedic evaluation.
Check the elbow for stability by fully flexing and extending the elbow while pronating and supinating the forearm. These movements should be easy after reduction.
Perform post-procedure radiographs to confirm proper reduction and identify any coexisting fractures.
Immobilize the elbow at approximately 90° of flexion with the forearm in the neutral position or pronation in a posterior long arm splint. Do not use a circumferential cast.
Observe patient for 2 to 3 hours. Patients with significant soft tissue swelling, hematoma, or questionable vascular/neurologic integrity should be admitted for continuing observation, either to an emergency department observation unit or to a hospital. Arrange this with the orthopedic surgeon.
If the patient is discharged to home, arrange follow-up care with the orthopedic surgeon and instruct the patient to return if swelling worsens, for progressively increasing severe pain, or if the digits develop cyanosis, coolness, weakness, or paresthesias.
Tips and Tricks for Posterior Elbow Dislocation Reduction
A widening between the distal humerus and the olecranon on radiographs indicates a higher risk for a vascular injury.
Drug Information for the Topic