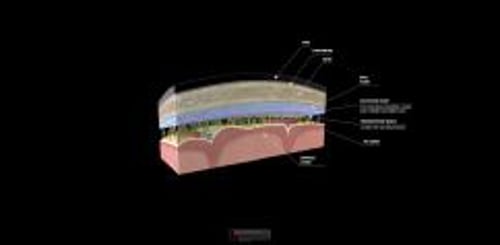
Meningitis is inflammation of the meninges and subarachnoid space. It may result from infections, other disorders, or reactions to medications. Severity and acuity vary. Findings typically include headache, fever, and nuchal rigidity. Diagnosis is by cerebrospinal fluid (CSF) analysis. Treatment includes antimicrobial medications as indicated plus adjunctive measures.
(See also Introduction to Brain Infections and Neonatal Bacterial Meningitis.)
Meningitis may be classified as acute, subacute, chronic, or recurrent. It may also be classified by its cause: bacteria, viruses, fungi, protozoa, or, occasionally, noninfectious conditions. But the most clinically useful categories of meningitis are
Meningeal inflammation as an atypical reaction to anti-inflammatory, immunosuppressive, or other medications
Acute bacterial meningitis is a particularly serious and rapidly progressive medical emergency requiring immediate administration of antibiotics. Viral and noninfectious meningitides are usually self-limited. Subacute and chronic meningitides usually follow a more indolent course than other meningitides, but determining the cause can be difficult.
Aseptic meningitis, an older term, is sometimes used synonymously with viral meningitis; however, it usually refers to acute meningitis caused by anything other than the bacteria that typically cause acute bacterial meningitis. Thus, aseptic meningitis can be caused by
Viruses
Noninfectious conditions (eg, medications, disorders)
Occasionally, other organisms (eg, Borrelia burgdorferi in Lyme disease, Treponema pallidum in syphilis)
Symptoms and Signs of Meningitis
Symptoms and signs of the different types of meningitis may vary, particularly in severity and acuity. However, all types tend to cause the following (except in infants and sometimes in patients who are very old or immunosuppressed):
Headache
Fever
Nuchal rigidity (meningismus)
Patients may appear lethargic or obtunded.
Nuchal rigidity, a key indicator of meningeal irritation, is resistance to passive or volitional neck flexion. Nuchal rigidity may take time to develop. Clinical tests for it, from least to most sensitive, are
Kernig sign (pain or resistance with passive extension of the patient's knees past 135 degrees in the setting of meningeal irritation)
Brudzinski sign (full or partial flexion of the hips and knees when the neck is flexed)
Difficulty touching the chin to the chest with the mouth closed
Difficulty touching the forehead or chin to the knee
Nuchal rigidity can be distinguished from neck stiffness due to cervical spine osteoarthritis or influenza with severe myalgia; in these disorders, neck movement in all directions is usually affected. In contrast, nuchal rigidity due to meningeal irritation affects mostly neck flexion; thus, the neck can usually be rotated but cannot be flexed.
Diagnosis of Meningitis
Cerebrospinal fluid (CSF) analysis
Meningitis is diagnosed mainly by CSF analysis. Because meningitis can be serious and lumbar puncture is a safe procedure, lumbar puncture should usually be done if there is any suspicion of meningitis. CSF findings differ by the type of meningitis but can overlap. (See table .)
If patients have signs suggesting increased intracranial pressure or a mass effect (eg, focal neurologic deficits, papilledema, deterioration in consciousness, seizures, especially if patients have HIV infection or are immunocompromised), neuroimaging—typically, contrast-enhanced CT or MRI—is done before lumbar puncture. In patients with increased intracranial pressure, lumbar puncture may cause brain herniation, usually within hours of the procedure.
Also, if a bleeding disorder is suspected, lumbar puncture is not done until the bleeding disorder is excluded or controlled.
When lumbar puncture is deferred, blood cultures should be obtained at the time of empiric treatment with antibiotics. After intracranial pressure has been lowered and if no mass is detected, lumbar puncture can be done.
If the skin over the putative spinal needle insertion site is infected or if a subcutaneous or parameningeal lumbar infection is suspected, the needle is inserted at a different site, usually into the cisterna magna or the upper cervical spine at C2 using radiologic guidance.
Treatment of Meningitis
Antimicrobial therapy as indicated
Adjunctive treatments
Infectious meningitis is treated with antimicrobial therapy as indicated clinically.
Adjunctive treatments for meningitis can include
Supportive measures
Treatment of complications or of associated disorders
Removal of causative medications
For bacterial meningitis, corticosteroids