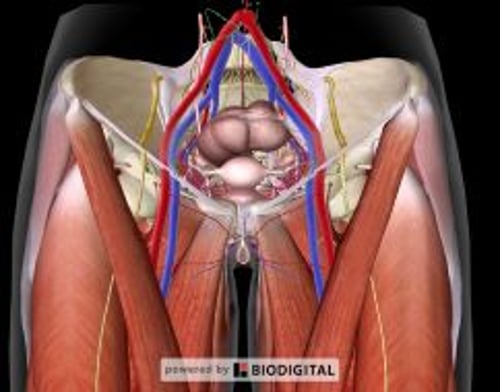
Percutaneous cannulation of the femoral vein uses anatomic landmarks to guide venipuncture and a Seldinger technique to thread a central venous catheter through the femoral vein and into the inferior vena cava.
Femoral venous cannulation is frequently used as initial central venous access in resuscitations. It has the procedural advantages of a relatively superficial and easily accessed vein. In addition, the nearby anatomy lacks the complexity and vital structures of the jugular and subclavian regions. However, femoral central venous catheters (CVCs) have higher risks of infection and thrombosis and should be removed as soon as possible when alternate vascular access is available.
Ultrasound guidance for placement of femoral lines increases the likelihood of successful cannulation and reduces the risk of complications. When ultrasound guidance and trained personnel are available, this method of placement is preferred.
(See also Vascular Access: Central Venous Catheterization and How To Do Femoral Vein Cannulation, Ultrasound-Guided.)
Indications for Femoral Vein Cannulation
Secure or long-term venous access that is not available using other sites
Inability to obtain peripheral venous access or intraosseous infusion
IV infusion of fluids and medications for patients in cardiac arrest
IV infusion of medications that may be irritating to veins when administered peripherally (eg, high-concentration fluids, chemotherapy, vasopressors, parenteral nutrition)
IV infusion of high flows or large fluid volumes if placement of large-bore (eg, 18- or 16-gauge) peripheral venous catheters or other CVCs is not feasible
Transvenous cardiac pacing or pulmonary arterial monitoring (Swan-Ganz catheter)*
Placement of inferior vena cava filter
Need for central venous access in patients with superior vena cava syndrome
Central venous access above the diaphragm, unless contraindicated, is generally preferred to femoral venous access in patients who require central venous access. Femoral lines are usually used only as provisional access because they have a high risk of infection. They should be exchanged for lines above the diaphragm as soon as possible.
* For transvenous cardiac pacing and pulmonary arterial monitoring, a right internal jugular cannulation or a left subclavian vein cannulation typically is preferred.
Contraindications to Femoral Vein Cannulation
Absolute contraindications
Intra-abdominal hemorrhage or pelvic trauma
Femoral vein thrombosis
Local infection at the insertion site
Antibiotic-impregnated catheter in a patient with an allergy to the specific antibiotic
For intra-abdominal hemorrhage or pelvic trauma, sites that drain into the superior vena cava should be used.
Relative contraindications
Coagulopathy, including thrombocytopenia or anticoagulant medications (including antiplatelet medications)*
Local anatomic distortion (traumatic or congenital), or gross obesity
History of prior catheterization of the femoral vein (prior catheterization may have resulted in scar tissue formation making catheter placement more difficult)
Uncooperative patient (should be sedated if necessary)
Ambulatory patient
* Anticoagulant medications (eg, for atrial fibrillation) increase the risk of bleeding with femoral vein cannulation, but this risk must be balanced against the increased risk of thrombosis (eg, stroke) if anticoagulation is reversed. Discuss any contemplated reversal with the clinician managing the patient's anticoagulation and then with the patient. Femoral vein cannulation may be preferred for patients with coagulopathies because, unlike the subclavian sites, the femoral triangle is readily compressible and vital structures (airway, pleural dome, mediastinum, blood vessels to brain) are distant from the venipuncture site.
Complications of Femoral Vein Cannulation
(See also Complications of central venous catheterization.)
Potential complications include
Infection
Thrombosis
Arterial puncture
Hematoma
Retroperitoneal bleeding
Damage to the vein
Air embolism
Catheter misplacement*
Nerve damage
Arteriovenous fistula formation (rare)
Bladder or bowel perforation (rare)
* Rare complications due to femoral catheter misplacement include arterial catheterization and retroperitoneal infusion.
Guidewire or catheter embolism also rarely occurs.
To reduce the risk of venous thrombosis and central line-associated bloodstream infection (CLABSI), CVCs should be removed as soon as they are no longer needed.
Equipment for Femoral Vein Cannulation
Sterile procedure, barrier protection
Antiseptic solution (eg, chlorhexidine-alcohol, chlorhexidine, povidone-iodine, alcohol)Antiseptic solution (eg, chlorhexidine-alcohol, chlorhexidine, povidone-iodine, alcohol)
Sterile drapes (large), towels
Sterile hats, masks, gowns, gloves
Face shields
Seldinger (catheter-over-guidewire) technique
Cardiac monitor
Local anesthetic (eg, 1% lidocaine without epinephrine, approximately 5 mL)Local anesthetic (eg, 1% lidocaine without epinephrine, approximately 5 mL)
Small anesthetic needle (eg, 25 to 27 gauge, 3 cm [approximately 1 inch] long)
Large anesthetic/finder* needle (22 gauge, 4 cm [approximately 1.5 inches] long)
Introducer needle (eg, thin-walled, 18 or 16 gauge, with internally beveled hub, 6 cm [approximately 2.5 inches] long)
3- and 5-mL syringes (use slip-tip syringes for the finder and introducer needles)
Guidewire, J-tipped
Scalpel (#11 blade)
Dilator
Central venous catheter (adult: 8 French or larger, minimum length for femoral catheter is 24 cm [approximately 9.5 inches])
Sterile gauze (eg, 10 × 10 cm [4 × 4 inch] squares)
Sterile saline for flushing catheter port or ports
Nonabsorbable nylon or silk suture (eg, 3-0 or 4-0)
Chlorhexidine patch, transparent occlusive dressingChlorhexidine patch, transparent occlusive dressing
* A finder needle is a thinner needle used for locating the vein before inserting the introducer needle. It is not typically used but is optional (eg, in patients with obesity) for femoral vein cannulation.
Having 1 or 2 assistants is helpful.
Additional Considerations for Femoral Vein Cannulation
Cannulation attempts sometimes fail. Do not exceed 2 or 3 attempts (which increases the risk of complications), and use new equipment with each attempt (ie, do not re-use needles, catheters, or other equipment because they may have become blocked with tissue or blood).
During cardiopulmonary arrest, or even low blood pressure and hypoxia, arterial blood may be dark and not pulsatile and may be mistaken for venous blood.
If the femoral artery is errantly cannulated by either the tissue dilator or the CVC, leave the dilator or catheter in place and obtain surgical consultation for possible surgical removal.
Relevant Anatomy for Femoral Vein Cannulation
The femoral vein and artery are accessible within the femoral triangle, which is defined by the inguinal ligament superiorly, the adductor longus muscle medially, and the sartorius muscle laterally.
The inguinal ligament spans between the symphysis pubis and the anterior superior iliac spine.
The femoral artery is palpated inferior to the inguinal ligament, typically at or just medial to its midpoint. In the absence of a palpable femoral pulse, the femoral artery is presumed to lie in this region.
The femoral vein lies medially adjacent to the femoral artery. With increasing distance from the inguinal ligament, the vein runs under the artery.
The desired point of femoral vein puncture is 1 to 2 cm inferior to the inguinal ligament. Bleeding due to a vascular impalement here can be controlled by externally compressing the vessels against the femoral head.
The retroperitoneal space lies superior to the inguinal ligament. Bleeding due to a vascular impalement here causes retroperitoneal bleeding, and external compression of the vessels may be impossible.
Positioning for Femoral Vein Cannulation
Raise the bed to a comfortable height for you (ie, so you may stand straight while doing the procedure).
Place the patient supine.
Abduct and externally rotate the leg.
Retract a pannus or a urethral catheter away from the inguinal area using tape (or an assistant if needed).
Step-by-Step Description of Femoral Vein Cannulation
Do a preliminary inspection (nonsterile) to identify the symphysis pubis, anterior superior iliac crest, femoral pulse, and umbilicus.
Attach the cardiac monitor to the patient and turn it on.
Excess hair may be clipped but not shaved from the site. Shaving increases the risk of infection.
Prepare the equipment
Place sterile equipment on sterilely covered equipment trays.
Use appropriate personal protective equipment.
Draw the local anesthetic into a syringe.
Optional: Attach a finder needle to a 5-mL syringe with 1 to 2 mL of sterile saline in it.
Attach the introducer needle to a 5-mL syringe with 1 to 2 mL of sterile saline in it. Align the bevel of the needle with the volume markings on the syringe.
Pre-flush all lines of the CVC with 3 to 5 mL of sterile saline and then close the ports with caps or syringes.
When flushing a central line, use a 10-mL syringe (or one of equal or greater diameter) and do not push too hard to avoid rupturing the line.
Prepare the sterile field
Swab a broad area of skin with antiseptic solution, from the anterior superior iliac spine to the midline and extending down 15 cm below the inguinal ligament.
Allow the antiseptic solution to dry for at least 1 minute.
Place sterile towels around the site.
Place large sterile drapes (eg, a full-body drape) to establish a large sterile field.
Put on sterile mask and hat.
Put on sterile gown and gloves.
Establish the needle insertion path
Gently palpate the femoral arterial pulse using 2 or 3 fingers. Palpate gently so as not to compress the adjacent femoral vein (a compressed venous lumen is difficult to access).
The needle insertion path: Insert procedural needles (local anesthetic, finder, and introducer needles) 2 to 4 cm inferior to the inguinal ligament, 1 cm medial to the femoral artery, at a 45 to 60° angle into the skin, and aim toward the umbilicus.
Maintain femoral artery palpation during needle insertions and keep the needle medial to the artery to avoid impaling the artery.
Anesthetize the cannulation site
Place a wheal of anesthetic at the needle entry site and then inject anesthetic into the skin and soft tissues along the anticipated needle insertion path. Maintain gentle negative pressure on the syringe plunger as you advance to identify intravascular placement and prevent an intravascular injection.
If blood returns into the syringe, stop advancing the needle, hold the syringe in place, and now regard this needle as a finder needle. Proceed to Assess the blood return below.
Insert the introducer needle (or finder needle, optional)
Insert the introducer needle (or, optionally, finder needle), with the bevel facing up, along the needle insertion path.
Maintain gentle negative pressure on the syringe plunger as you advance the needle.
Stop advancing when a flash of blood appears in the barrel of the syringe (you may feel the needle pop through the wall as it enters the lumen). Hold the syringe motionless in this spot. Even a slight movement may displace the needle tip from the vein.
If no flash of blood appears in the barrel after 2 to 4 cm of insertion, withdraw the needle slowly. If the needle had initially passed completely through the vein, a flash may now appear as you withdraw the needle tip back into the lumen. If a flash still does not appear, withdraw the needle almost to the skin surface, change direction, and try again to advance the needle into the vein. Do not change direction of the needle while it is fully inserted.
Assess the blood return
Continue to hold the syringe motionless.
Securely grasp the needle hub, and also hold it motionless.
Remove the syringe from the needle hub and briefly let blood flow out to confirm that the blood is venous (ie, dark red and flowing but not pulsatile). Then immediately cover the hub with your thumb to stop the blood flow and prevent air embolism.
However, if the blood is bright red and pulsatile (arterial), terminate the procedure. Remove the needle and use sterile gauze for 10 minutes to hold external pressure on the area and to help prevent bleeding and hematoma.
Optional: Use the finder needle to guide insertion of the introducer needle
If up to this point you have been inserting a finder needle (or an anesthetic needle that found the vein), now you will use this needle to guide insertion of the introducer needle.
Hold the introducer syringe with the needle bevel facing up.
Use 1 of 2 insertion methods: Either remove the finder needle and immediately insert the introducer needle along the same path, or keep the finder needle in place and insert the introducer needle underneath and roughly parallel to it (at a slightly shallower angle to the skin).
Stop advancing the introducer needle and hold it motionless when a flash of blood appears in the barrel of the syringe.
If the finder needle has not been removed, remove it now.
Assess blood flow from the introducer needle as described in Assess the blood return above.
Insert the guidewire
Continue to hold the introducer needle motionless.
Insert the J-curved end of the guidewire into the introducer needle, with the J curve facing up.
Advance the guidewire through the needle and into the vein. Do not force the wire; it should slide smoothly. Advance the wire 20 to 30 cm.
If you feel any resistance as you advance the guidewire, stop advancing it. Try to gently withdraw the wire slightly, rotate it slightly, and then re-advance it, or try to gently withdraw the wire entirely, reestablish the needle tip within the vein (confirmed by venous blood return), and then reinsert the wire.
However, if you feel any resistance as you withdraw the wire, terminate the procedure and withdraw the needle and guidewire together as a unit (to prevent the needle tip from shearing through the guidewire within the patient). Then use gauze squares for 10 minutes to hold external pressure on the area and to help prevent bleeding and hematoma.
Once the guidewire has been inserted, continue to hold it securely in place with one hand and maintain control of it throughout the remainder of the procedure.
Remove the introducer needle (after successful guidewire insertion)
First, securely hold the guidewire distal to the needle and pull the needle from the skin.
Then, securely hold the guidewire at the skin surface and slide the needle down the remaining length of the guidewire to remove the needle.
Widen the insertion tract
Extend the skin insertion site: Using the scalpel, make a small stab incision (approximately 4 mm) into the skin insertion site, avoiding contact with the guidewire, to enlarge the site and allow it to accommodate the larger diameters of the tissue dilator and the catheter.
Advance the tissue dilator over the guidewire: First, grasp the guidewire at the skin and slide the dilator down the length of the wire to the skin. Then grasp the wire just distal to the dilator, hold the dilator near the skin surface, and use a corkscrew motion as needed to stepwise insert the entire length of the dilator. Maintain your grasp on the guidewire at all times during the insertion.
If there is resistance at the level of the skin when advancing the tissue dilator over the guidewire, slightly enlarge the skin incision with the scalpel before advancing the tissue dilator over the guidewire again to avoid inadvertently bending the guidewire.
Remove the dilator: First, securely hold the guidewire distal to the dilator and pull the dilator from the skin. When the guidewire is visible at the skin surface, completely remove the dilator by sliding it down the remaining length of the guidewire.
Place the catheter
Advance the catheter over the guidewire to the skin surface: Hold the guidewire fixed at the skin surface, thread the catheter tip over the distal end of the guidewire, and slide the catheter down to the skin surface at a 45° angle. The distal end of the guidewire should now be protruding from the port hub.
If the distal end of the guidewire is not protruding from the port hub, incrementally advance the guidewire outward from the skin surface while holding the catheter tip close to the surface until the guidewire protrudes.
Continue to advance the catheter into the vein: Grasp and control the guidewire where it protrudes from the hub. Hold the catheter near its tip and insert the tip through the skin. Then, in increments of several centimeters and using a corkscrew motion as necessary, stepwise advance the entire length of the femoral catheter.
Maintain your grasp on both the guidewire and the catheter.
Remove the guidewire: Withdraw the guidewire while holding the catheter securely in place at the skin surface.
Flush each catheter port with saline: First, draw any air from the line and confirm venous blood flow into the hub. Then, using a 10-mL syringe (or one of equal or greater diameter) and without using excessive force, push 20 mL of saline into the line to clear it.
Dress the site
If the patient is awake or minimally sedated, use 1% lidocaine to anesthetize the skin at the planned suture locations.If the patient is awake or minimally sedated, use 1% lidocaine to anesthetize the skin at the planned suture locations.
Place a chlorhexidine-impregnated disk on the skin at the catheter insertion point. Place a chlorhexidine-impregnated disk on the skin at the catheter insertion point.
Suture the skin to the mounting clip on the catheter.
To prevent pulling on the insertion site, suture the catheter at a second site so that a curved or looped segment of catheter lies between the 2 sites.
Apply a sterile occlusive dressing. Transparent membrane dressings are commonly used.
Warnings and Common Errors for Femoral Vein Cannulation
Never lose grasp of the guidewire.
During cardiopulmonary arrest, or even low blood pressure and hypoxia, arterial blood may be dark and not pulsatile and may be mistaken for venous blood.
To help prevent air embolism, CVCs should be inserted (and removed) with the vascular cannulation site positioned dependant to the heart.
Tips and Tricks for Femoral Vein Cannulation
Femoral lines are usually used only as provisional access because they have a high risk of infection. They should be exchanged for lines above the diaphragm as soon as possible.
Drug Information for the Topic